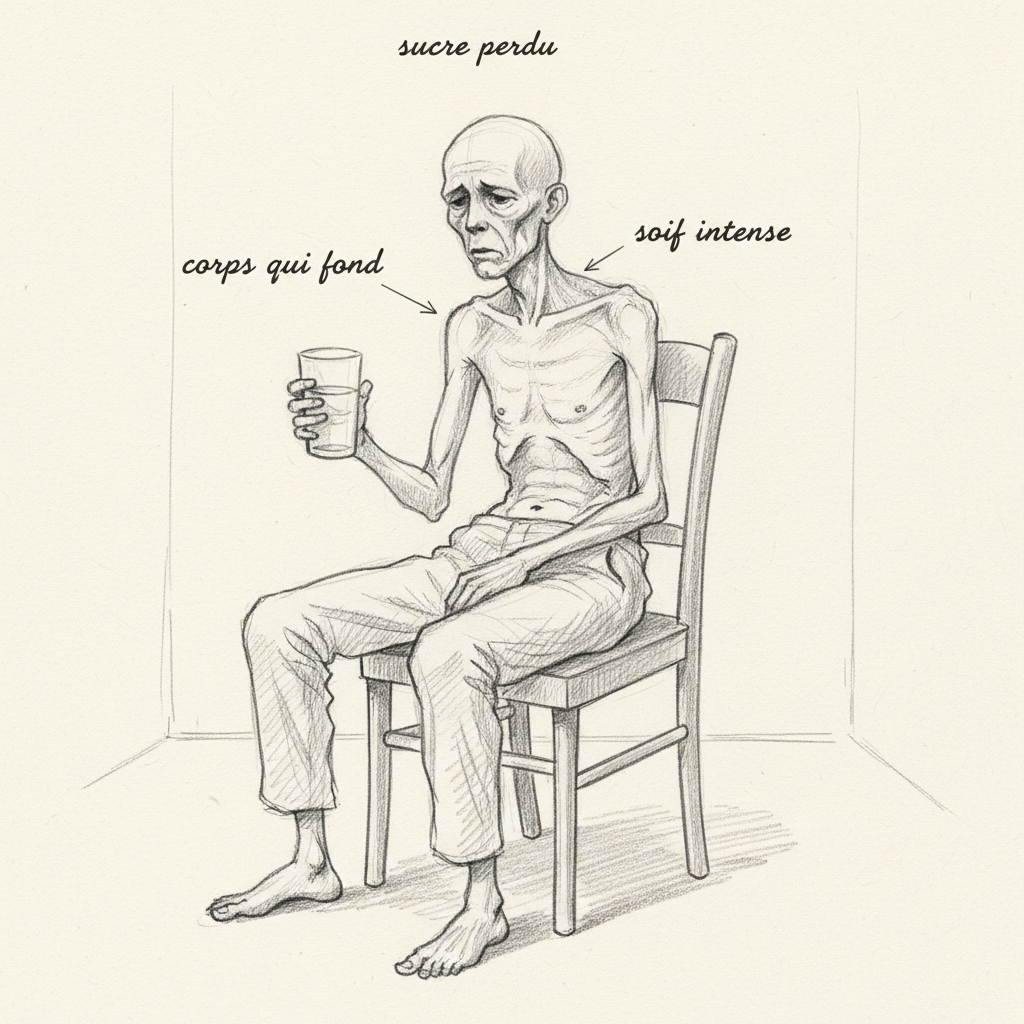
Alain lost eight kilos in two months without trying. At sixty-two years old, after a lifetime of good living, he sees his pants hanging loose and his arms thinning. He drinks liters of water without ever quenching his thirst. He gets up three times a night to urinate. He is permanently tired, with a muscle weakness that surprises him when he climbs stairs. His doctor finally tested his blood glucose: 2.4 g/L. Alain is diabetic. His pancreas has given up.
Alain’s story is that of millions of people. For years, his pancreas overproduced insulin to compensate for the growing resistance of his cells (the hyperinsulinism). Then, after years of overwork, the beta cells of the islets of Langerhans became exhausted. Insulin production dropped. Glucose accumulated in the blood without being able to enter the cells. This is the transition from insulin resistance to confirmed type 2 diabetes: the stage of pancreatic exhaustion.
From surplus to shortage: the trajectory of the pancreas
The trajectory is predictable and documented. Phase 1: diet rich in refined carbohydrates and sedentary lifestyle gradually establish insulin resistance. The pancreas compensates by producing more. Phase 2: chronic hyperinsulinism sets in. The pancreas works overtime. Blood glucose remains normal thanks to this overproduction. Phase 3: beta cells become exhausted, oxidized, and die (apoptosis). Insulin production drops. Blood glucose rises. Diabetes develops.
This trajectory takes ten to twenty years. Throughout this entire period, fasting blood glucose often remains normal (the pancreas compensates). This is why diabetes is diagnosed late: when blood glucose rises, fifty percent of beta cells are already destroyed.
Signs of insulin insufficiency
Involuntary weight loss is the most serious warning sign. Without insulin, glucose circulates in the blood but cannot nourish the cells. The cells turn to reserves of fat (lipolysis) and muscle proteins (proteolysis) for energy. You lose weight, but you lose muscle and fat, not water.
Polyuria-polydipsia (urinating a lot and being permanently thirsty) is the classic syndrome. Excess glucose in the blood is filtered by the kidneys. When the kidney’s reabsorption capacity is exceeded (renal glucose threshold, around 1.8 g/L), glucose passes into the urine and carries water with it through osmosis. You urinate abundantly, you become dehydrated, you are thirsty. You drink, you urinate, you are thirsty: the cycle is vicious.
Intense fatigue and muscle weakness come from the cells’ inability to use glucose. They are starving amid plenty: glucose is everywhere in the blood but cannot enter the cells without the key (insulin).
Slow wound healing, blurred vision (crystalline lens edema from hyperglycemia), recurring infections (germs love glucose) and tingling in the extremities (early neuropathy) are signs of early complications.
Take the Hertoghe insulin deficiency test.
Causes of pancreatic exhaustion
Chronic hyperinsulinism is the main cause. Years of overproduction eventually exhaust beta cells. Oxidative stress inside the cell (metabolic overactivity generates free radicals) damages the mitochondrial DNA of beta cells and triggers apoptosis. Glucotoxicity (hyperglycemia itself is toxic to beta cells) and lipotoxicity (excess free fatty acids are toxic) accelerate destruction.
Autoimmunity plays a role in type 1 diabetes (destruction of beta cells by antibodies) and in LADA (Latent Autoimmune Diabetes of Adults), a slow form of autoimmune diabetes that develops after thirty years and is often confused with type 2 diabetes.
Zinc deficiency directly compromises insulin synthesis. Zinc is a structural component of insulin (two zinc atoms per insulin hexamer) and a cofactor in its secretion. Chromium deficiency reduces receptor sensitivity, forcing the pancreas to produce more. Magnesium deficiency impairs insulin signaling.
Supporting the pancreas naturally
Chromium is the most specific micronutrient. Chromium picolinate at 200 micrograms per day improves insulin receptor sensitivity and reduces the pancreas’s workload. Zinc bisglycinate at 15 milligrams per day supports insulin synthesis and secretion. Magnesium (300 mg per day) improves signaling.
Berberine (500 mg two to three times daily before meals) protects beta cells from oxidative stress and improves insulin sensitivity. Alpha-lipoic acid (300 to 600 mg per day) is an antioxidant that protects beta cells and improves peripheral sensitivity. Vitamin D (4000 IU per day) has receptors on beta cells and modulates insulin secretion.
Low glycemic load diet reduces insulin demand at each meal. Proteins and healthy fats first. Vegetables in abundance. Complex carbohydrates in moderate amounts (legumes, whole grains, sweet potatoes). Zero refined sugar, zero soda, zero fruit juice.
Physical exercise increases GLUT4 expression in muscles, allowing glucose to enter without insulin. Thirty minutes of walking after each meal. Strength training two to three times per week to increase muscle mass that consumes glucose.
Important: confirmed hypo-insulinism with elevated blood glucose requires medical monitoring. Naturopathy supports but does not replace medical diabetes treatment. Metformin, GLP-1 analogs and insulin therapy have their place when the pancreas is too exhausted to be naturally stimulated. The naturopathic objective is to intervene upstream, during the resistance phase, to prevent exhaustion.
For further reading
- Hyperinsulinism: when excess insulin makes you gain weight and fatigue
- Myo-inositol: mood, blood glucose and ovaries in one molecule
- Thyroid and weight: why you don’t lose weight despite everything
- Vitamin B8 (biotin): hair, skin and blood glucose in one molecule
Sources
- Hertoghe, Thierry. Atlas of Hormonal and Nutritional Medicine. International Medical Books, 2006.
- Curtay, Jean-Paul. Nutritherapy: scientific bases and medical practice. Testez Éditions, 2016.
- Mouton, Georges. Digestive Ecology. Marco Pietteur, 2004.
If you want personalized support, you can book a consultation.
Healthy Recipe: Dried fruit-cinnamon porridge: Cinnamon helps regulate blood glucose.



Laisser un commentaire
Sois le premier à commenter cet article.