Thomas is forty-one years old. An executive at a consulting firm, he has been working sixty hours a week for five years. When he sat down across from me, his hands were trembling slightly. He told me he had been sleeping poorly for eight months, that he had palpitations when opening his email in the morning, and that the previous week he had found himself unable to write a simple meeting report. He who managed projects worth several million euros could no longer find his words in front of a Word document. His doctor had prescribed him an anxiolytic and two weeks off. Thomas looked at me with that expression I know well, the one people have when they don’t understand what’s happening to them, and he asked me the question I hear at least twice a week: “How did I get here? I’ve never been fragile.”
Thomas is not fragile. His brain has simply switched into an archaic mode of functioning that has nothing to do with fragility. A survival mode. And it is precisely this shift—silent, progressive, biochemical—that no one has ever explained to him.
You think burnout is working too much. Neurobiology says it’s your brain that can no longer tell the difference between an urgent email and a tiger.
“It is not things themselves that disturb people, but their judgments about those things.” Epictetus, quoted by Dr. Anne Lucas1
Stress: a hijacked survival mechanism
The word “stress” was introduced to biology by Hans Selye in 1936. Before him, the term belonged to materials physics. Selye borrowed it to describe the non-specific response of an organism to any demand. And he identified three successive phases that make up the general adaptation syndrome2.
The first phase is alarm. The organism perceives a threat. The adrenal glands release adrenaline and noradrenaline. The heart accelerates. Muscles tense. Breathing speeds up. Pupils dilate. Blood is redirected toward muscles at the expense of the digestive tract. This is the fight-or-flight response, programmed for millions of years to flee a predator or confront an enemy. This phase is brief, intense, and normally followed by a return to calm.
The second phase is resistance. If stress persists, the organism adapts. The adrenal glands shift from adrenaline to cortisol, a hormone that maintains energy at an elevated level over time. Cortisol mobilizes glucose reserves, slows the immune system, maintains blood pressure. It’s a remarkable adaptation mechanism. But it has a cost. As I detail in the article on stress, cortisol and the thyroid, chronically elevated cortisol diverts pregnenolone at the expense of progesterone and DHEA, blocks the conversion of T4 to active T3, promotes the production of reverse T3, and depletes reserves of magnesium, zinc, B vitamins and vitamin C. The body holds, but it empties.
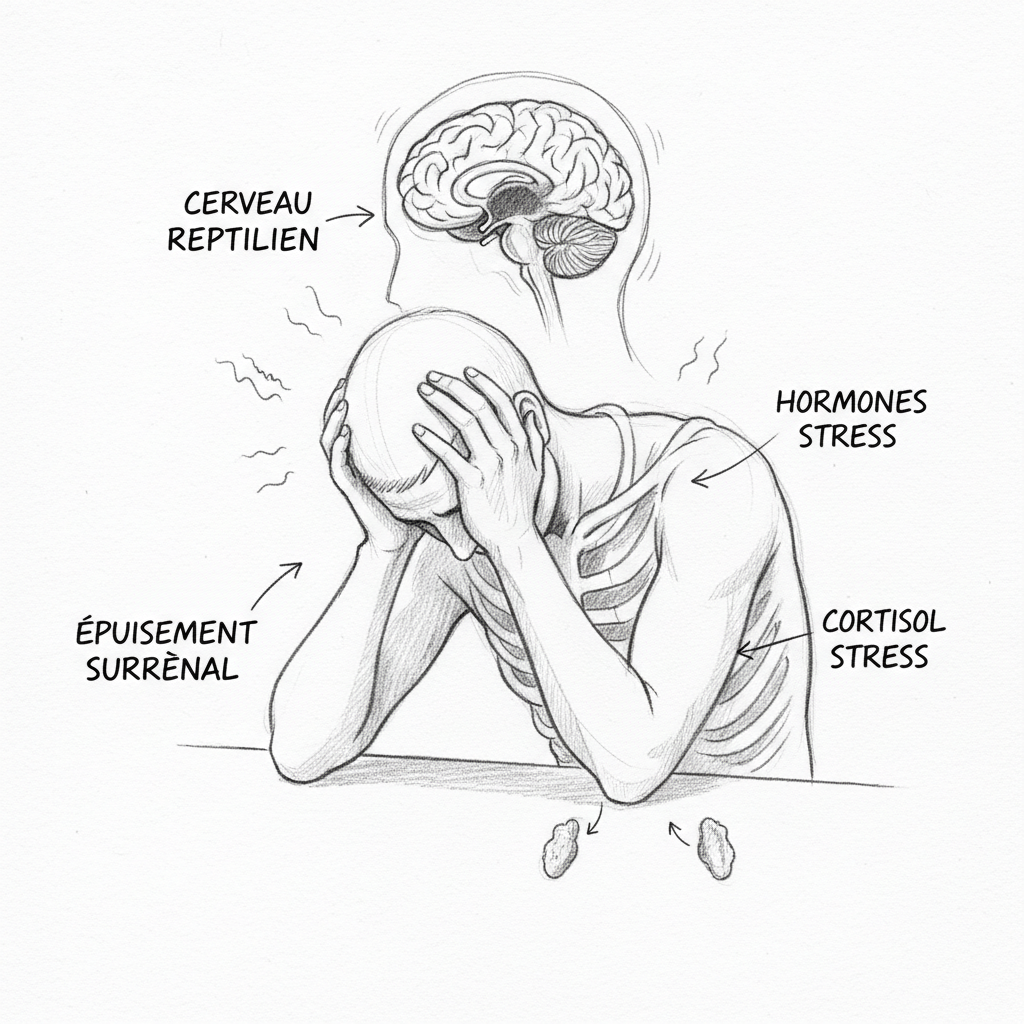
The third phase is exhaustion. The adrenal glands can no longer keep up. Cortisol collapses. This is burnout in the biological sense. The organism no longer has the resources to maintain resistance. Everything fails at once: energy, sleep, concentration, immunity, motivation. This is the phase that Selye considered potentially fatal. And it’s the phase Thomas was in when he came to my office.
The difference between stress and burnout is the difference between a sprint and a marathon run at sprint speed. The first is normal. The second is a metabolic catastrophe. If you want to understand in detail the three stages of adrenal exhaustion and how to identify them, I’ve written a complete article on the subject.
Laborit and the three states of instinctual emergency
Henri Laborit, a French neurobiologist and surgeon, published in 1986 a model that remains strikingly relevant for understanding burnout. Laborit describes three states of instinctual emergency, three archaic responses of the brain to threat3.
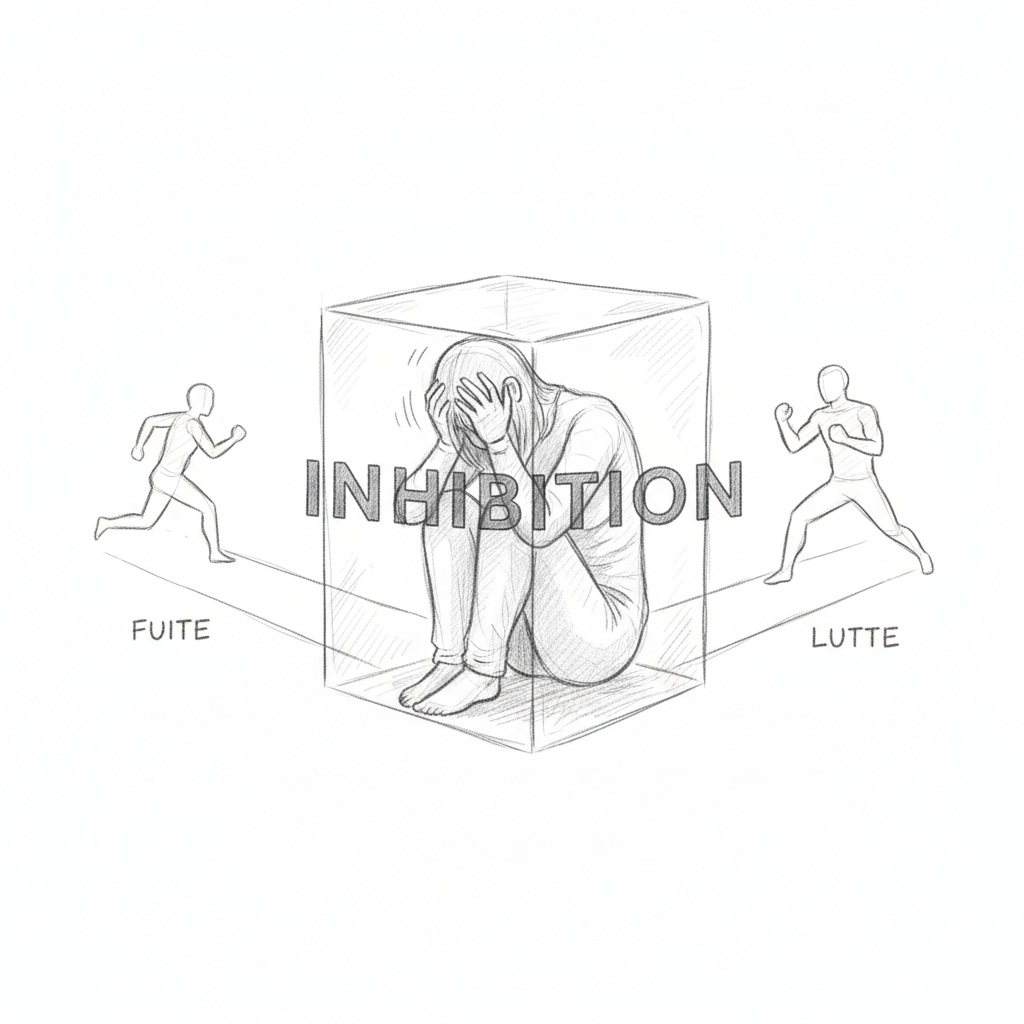
The first state is flight. The organism perceives danger and chooses to move away. It’s the response most economical in energy. Heart rate accelerates, adrenaline rises, muscles prepare. In a work situation, flight manifests as avoidance: you put off the difficult meeting, you stop reading your emails, you procrastinate on heavy files. This isn’t laziness. It’s a brain trying to flee what it perceives as a predator.
The second state is fight. The organism faces the threat. Cortisol rises, aggressiveness increases, tolerance decreases. In a company, fighting translates into disproportionate irritability, conflicts with colleagues, terse email responses, nocturnal bruxism (clenching teeth during sleep is a residue of combat behavior). Thomas clenched his teeth so hard at night that his dentist had to make him a mouthguard. Nobody had connected it to his work stress.
The third state is inhibition of action. This is the one Laborit considered most destructive. When you can neither flee nor fight, the brain freezes. The parasympathetic system takes over. Blood pressure drops. Heart rate slows. Energy collapses. The individual “disconnects.” In advanced burnout, inhibition manifests as a sense of emptiness, inability to make decisions, depersonalization (feeling like you’re watching yourself live from outside), and sometimes complete shock at tasks that were once simple. Thomas, unable to write his report, was in full inhibition of action.
Laborit understood it forty years ago: inhibition of action is the breeding ground for illness. When the body can neither act nor flee, it somatizes. Chronic muscle tensions, digestive problems, headaches, recurrent infections are not coincidences. They are the biological consequences of a brain stuck in inhibition, a brain that has locked all the exits.
The four territories of the brain: the ANC model
The neurocognitive and behavioral approach (ANC), developed by Dr. Jacques Fradin, proposes a functional model of the brain that remarkably illuminates the mechanism of burnout. This model distinguishes four territories, each with a specific function and a radically different mode of processing information4.
The first territory is the reptilian brain. It’s the oldest in evolutionary terms. It manages individual survival. Its vocabulary is binary: danger or no danger. Its responses are Laborit’s three states: flight, fight, inhibition. It doesn’t think. It doesn’t nuance. It reacts. Its processing speed is lightning-fast, a few milliseconds, because in survival situations, speed trumps accuracy. When a tiger appears, you don’t make a pros and cons list. You run. The problem is that your reptilian brain doesn’t distinguish between a tiger and an email from your boss on Sunday evening. The biochemical response is the same: adrenaline, cortisol, muscle tensions, tachycardia, hot flushes.
The second territory is the paleolimbic brain. It manages the survival of the collective, gregarious positioning, self-affirmation within the group. It’s the brain of social hierarchy, competition, submission, dominance. In a company, it’s permanently activated: the meeting where you must defend your project, your boss’s gaze, comparison with colleagues, fear of losing your place. The paleolimbic pushes you to prove your worth, to show that you’re coping, to absolutely not admit your fatigue. It’s what makes you say “I’ve got this” when you really don’t.
The third territory is the neolimbic brain. It manages the simple and the known. It’s the autopilot, the territory of habits, routines, personality. It works through pattern recognition: if a situation resembles something already experienced, it applies the solution it knows. This is extremely efficient for repetitive tasks and familiar situations. But it’s also a trap. The neolimbic is rigid. It hates novelty, uncertainty, change. And when a new situation arises, it does something catastrophic: it treats it as if it were known.
The fourth territory is the prefrontal neocortex. It’s the most recent in evolutionary terms, the most sophisticated, and the one that distinguishes us most from other mammals. It manages the complex and the unknown in adaptive mode. It’s capable of open-mindedness, nuance, creativity, perspective, innovation. It’s the territory of flexible thinking, problem-solving, informed decision-making. The prefrontal doesn’t react. It responds. And this difference between reacting and responding is at the heart of everything that distinguishes adaptive stress from pathological stress.
The autopilot trap: how stress arises in the brain
Dr. Anne Lucas, in her course at the DU of Micronutrition, describes the mechanism of stress according to the ANC model with a clarity that deserves to be detailed step by step5.
Everything begins with a new situation. An unexpected event, an unusual request, a change in schedule, a relational conflict. This situation arrives at the brain and the first question is: is it simple or complex? Known or unknown?
If the neolimbic judges the situation as simple and known, it activates the autopilot. It applies a preformatted response, a habit, a thought pattern from past experience. The problem occurs when this assessment is wrong. When the situation is actually complex or new, but the neolimbic treats it as if it were familiar. The automatic response is then inadequate. It doesn’t solve the problem. And that’s where the stress mechanism is triggered.
The prefrontal neocortex detects the error. It sees that the automatic response doesn’t work, that the situation isn’t resolved, that something is wrong. And it sends an alarm signal. But this signal doesn’t go back to the neolimbic to ask it to revise its assessment. It goes straight down to the reptilian brain. This is the fundamental short-circuit of stress. The reptilian receives an alarm signal that it interprets as a survival threat. And it triggers the cascade: adrenaline, cortisol, flight, fight or inhibition.
This mechanism explains why stress is so often disproportionate to the objective situation. You don’t stress because the situation is truly dangerous. You stress because your autopilot gave a wrong answer, your prefrontal detected it, and your reptilian interpreted this error signal as a vital danger. A mundane email can trigger an internal storm if the neolimbic classifies it as a “threat to my position,” and the prefrontal detects that your automatic response (ignore, or respond curtly) isn’t appropriate.
This is exactly what was happening to Thomas. Each new request, each unexpected meeting, each schedule change triggered his autopilot. And as the load became too complex for preformatted responses, the error signal looped back to the reptilian. Fifty, a hundred times a day, his reptilian brain received survival alarms. False alarms, but biochemically indistinguishable from real threats. His body produced cortisol as if he had to face a predator eight hours a day, five days a week, for five years.
The damage of chronic stress on the body
Autonomic nervous system (ANS) dysfunction is the first clinical marker of chronic stress. The ANS consists of two branches: the sympathetic system (accelerator) and the parasympathetic system (brake). In acute stress, the sympathetic dominates. In recovery phase, the parasympathetic regains control. In the burnout patient, this alternation is broken. The sympathetic remains permanently activated, or the organism shifts into a parasympathetic dominance of inhibition6.
The clinical signs of this dysregulation are numerous and often misinterpreted. Resting tachycardia, unexplained palpitations, hot flushes without hormonal cause, chronic muscle tensions (trapezius, jaw, solar plexus), nocturnal bruxism, cold sweats, transit problems (diarrhea or alternating constipation), loss or excess appetite, decreased libido, orthostatic dizziness, tinnitus, tension headaches. How many patients receive a beta-blocker for palpitations that are just the symptom of a reptilian brain on permanent alert.
Chronically elevated cortisol quietly destroys the body. It causes insulin resistance (cortisol maintains elevated blood glucose that eventually exhausts insulin receptors), abdominal weight gain (cortisol favors visceral storage), immunosuppression (cortisol inhibits T and B lymphocyte proliferation), bone demineralization (cortisol inhibits osteoblasts), muscle atrophy (cortisol is catabolic), and direct neurotoxicity to the hippocampus, the brain region responsible for memory and learning7. Thomas, who could no longer find his words, wasn’t suffering from early-onset dementia. His hippocampus was intoxicated by cortisol.
Cortisol systematically depletes reserves of magnesium, zinc, B vitamins (especially B5, B6, B9 and B12) and vitamin C. This creates an infernal vicious circle: stress depletes the nutrients necessary for neurotransmitter synthesis (dopamine, serotonin, GABA, noradrenaline), which makes the brain more vulnerable to stress, which depletes nutrients even more. It’s the downward spiral of burnout. And this is why micronutrition isn’t a luxury in burnout management. It’s a biochemical necessity.
Assessing your stress level: the tools science offers
Before talking about solutions, you need to know where you stand. Three scientifically validated assessment tools allow you to quantify your stress level and determine the severity of the situation8.
The first is the HAD questionnaire (Hospital Anxiety and Depression Scale). This questionnaire has fourteen items, seven for anxiety and seven for depression. The anxiety score is interpreted as follows: 0 to 7, normal state. 8 to 10, mild anxiety. 11 to 14, moderate anxiety. 15 to 21, severe anxiety. Dr. Lucas clarifies that HAD is a screening tool, not a diagnostic one. But an anxiety score above 10 should be a warning. And a score above 14 requires urgent intervention, often medical first.
The second is Cohen’s Perceived Stress Scale. It measures not the stressful events themselves but the subjective perception of stress. The score is interpreted as follows: below 25, no significant stress. Between 25 and 49, moderate stress. Above 50, pathological stress requiring intervention. The benefit of this scale is that it confirms the principle of Epictetus taken up by the ANC model: it’s not events that stress you, but the idea you have of them. Two people facing the same event can have diametrically opposite scores.
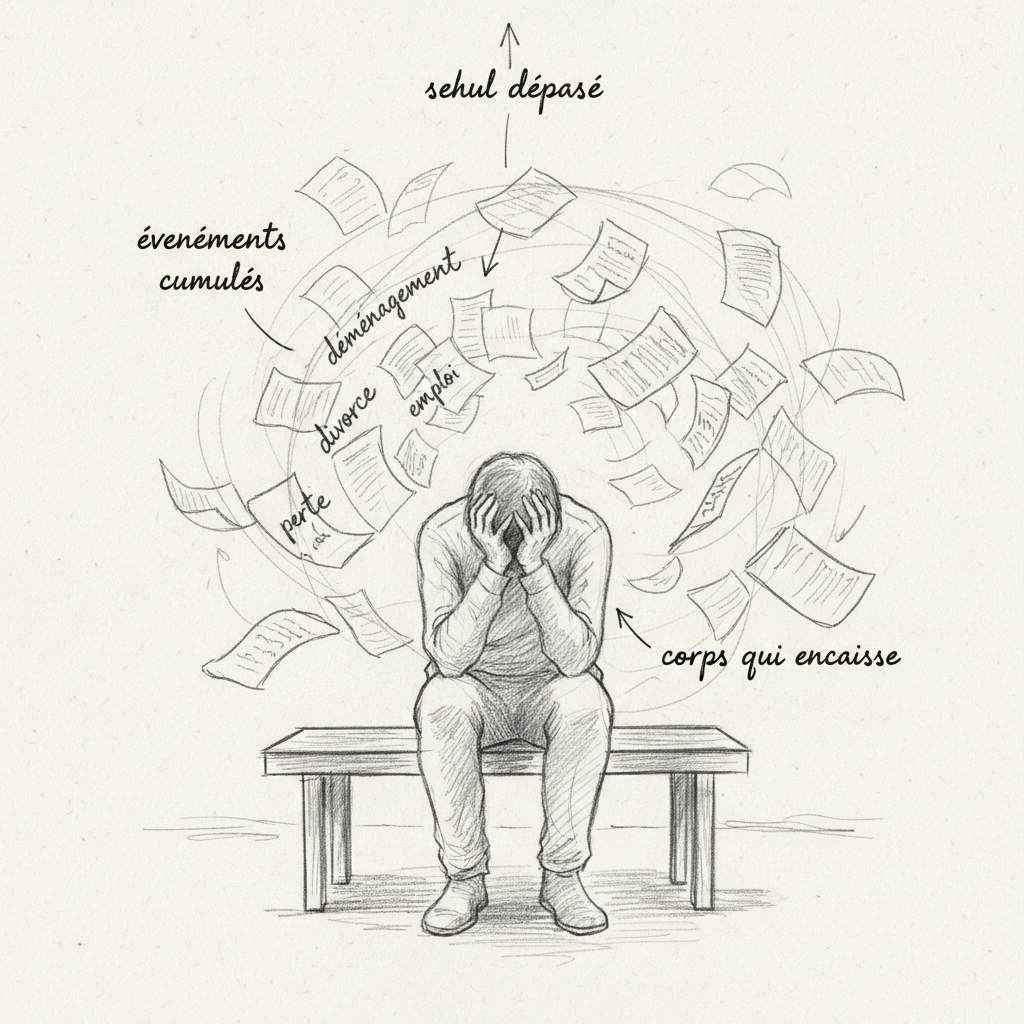
The third is the Holmes and Rahe scale, which dates from 1967 but is still used in clinical practice. It assigns a score to forty-three life events (death of a spouse: 100 points, divorce: 73, job loss: 47, relocation: 20, vacation: 13). You add up the scores of events experienced in the past twelve months. Below 150 points, the risk of illness in the following year is low. Between 150 and 300 points, the risk is moderate (about 50 %). Above 300 points, the risk exceeds 80 %9. Thomas accumulated 340 points: job change, birth of his second child, relocation, conflict with his management, and his father’s death six months earlier. Individually, each of these events was manageable. Combined, they overwhelmed his adaptive capacity.
I regularly use the Holmes-Rahe questionnaire in consultation to objectively assess my patients’ stress level. It’s a simple, quick tool, and it often opens eyes: many people don’t realize the accumulated stress over the past year until you put a number on it.
Exiting the reptilian: the prefrontal pathway
If the stress mechanism is a short-circuit of the reptilian, the solution is to restore access to the prefrontal. This is the fundamental principle of the neurocognitive approach: the prefrontal is the only territory capable of processing the complex and unknown without triggering an alarm10. It’s capable of stepping back, relativizing, finding creative solutions, accepting uncertainty without panicking.
But here’s the problem: when the reptilian is activated, access to the prefrontal is physiologically blocked. Cortisol inhibits the executive functions of the prefrontal cortex. This is a logical survival mechanism: when a tiger is chasing you, you don’t need to think, you need to run. But in chronic stress, this blockade becomes pathological. The reptilian locks the prefrontal, which can no longer send regulatory signals, which keeps the reptilian on alert, which locks the prefrontal even more. Closed loop.
To break this loop, you must act on two fronts simultaneously. The first is biochemical: restore reserves of magnesium, B vitamins, omega-3s and vitamin C to give the brain the raw materials needed for the synthesis of inhibitory neurotransmitters (GABA, serotonin) that calm the reptilian. The second is behavioral: deliberately practice techniques that activate the prefrontal and parasympathetic.
Physiological breathing (cardiac coherence, abdominal breathing) is the most powerful and fastest lever. The vagus nerve, which innervates the heart and digestive tract, is the main mediator of the parasympathetic system. Slow, deep breathing (six cycles per minute, meaning five seconds of inhalation and five seconds of exhalation) directly activates the vagus nerve and tips the sympathetic/parasympathetic balance in favor of the brake. Five minutes is enough to lower cortisol measurably. It’s a doorway to the prefrontal you can use anywhere, anytime.
Moderate physical exercise is the second lever. The article on sport and micronutrition details the mechanisms involved: increased BDNF (Brain-Derived Neurotrophic Factor), stimulation of hippocampal neurogenesis, increased serotonin and dopamine synthesis, endorphin release. Thirty minutes of brisk walking per day is enough. But be careful: intense, prolonged exercise increases cortisol. In burnout, the marathon is your enemy. Walking, yoga, swimming, cycling at moderate pace are your allies.
Sleep is the third lever, and probably the most neglected. As I explain in the article on sleeping well naturally, it’s during deep sleep that cortisol drops, growth hormone is secreted (tissue repair), memories are consolidated, and brain metabolic waste is eliminated via the glymphatic system. Burnout without sleep restoration is burnout that doesn’t heal. Melatonin, magnesium bisglycinate at bedtime, no screens an hour before bed, a cool and dark bedroom: these are the fundamentals.
The micronutritional protocol for chronic stress
Dr. Anne Lucas insists on a fundamental principle: in chronic stress, micronutrient needs explode while diet deteriorates (stress pushes toward fast sugar, coffee, alcohol, skipped meals)[^11]. Supplementation is not optional. It’s structurally necessary.
Magnesium is the absolute priority. It’s the first mineral depleted by cortisol. A magnesium deficit lowers the stress tolerance threshold, promotes muscle tensions, cramps, bruxism, irritability, sleep problems and palpitations. Magnesium bisglycinate is the best tolerated and best absorbed form, at 300 to 400 mg per day divided into two doses (morning and evening). The article on magnesium, thyroid and sleep details the interactions between these three systems.
B vitamins are the second pillar. B5 (pantothenic acid) is the cofactor for cortisol synthesis in the adrenal glands. B6 as pyridoxal-5-phosphate (P5P) is a cofactor for dopamine, serotonin and GABA synthesis. B9 (methylfolate) and B12 (methylcobalamine) are essential for methylation and homocysteine recycling. A B complex at physiological doses is the minimum. In advanced burnout, B6 P5P at 50 mg per day and B5 at 500 mg per day are often necessary[^12].
Omega-3 EPA and DHA protect neuronal membranes and exert powerful anti-inflammatory effects by modulating the AA/EPA ratio. As I detail in the article on omega-3s and membrane fluidity, DHA is the major structural component of brain membranes. An omega-3 deficit compromises neurotransmitter exocytosis and synaptic receptor mobility. Two to three grams of EPA/DHA per day is the typical dosage in chronic stress.
Vitamin C is the cofactor for cortisol synthesis (in the adrenal glands, vitamin C concentrations are among the highest in the body) and for the conversion of dopamine to noradrenaline. One to two grams per day, divided into multiple doses (vitamin C is water-soluble and eliminated quickly), support the adrenal axis without artificially stimulating it.
Zinc is a cofactor for pyridoxal kinase (enzyme that activates B6), delta-6-desaturase (key enzyme in omega-3 metabolism), and antioxidant enzymes (SOD). Chronic stress depletes zinc, which compromises downstream neurotransmitter synthesis and antioxidant protection. Fifteen to thirty milligrams of zinc bisglycinate per day away from meals completes the protocol.
Adaptogenic plants are the final stage of the rocket. Rhodiola (Rhodiola rosea) modulates the hypothalamic-pituitary-adrenal axis and increases stress resistance without excitant effects. Ashwagandha (Withania somnifera) lowers cortisol and improves sleep quality. Eleuthero (Eleutherococcus senticosus) supports cognitive performance under stress. These plants should be used in two to three month courses, not permanently, and never without first correcting underlying deficiencies[^13].
The intestine in burnout: the connection no one makes
Chronic stress destroys the intestine. This is not a metaphor. Cortisol alters intestinal permeability by degrading tight junctions between enterocytes. The enteric nervous system (the “second brain,” with its 200 million neurons) is directly connected to the central brain via the vagus nerve, and it bears the full brunt of ANS dysregulation. Intestinal motility is disturbed (hence bloating, constipation or alternating diarrhea). The microbiota becomes unbalanced (pathogenic bacteria proliferate under cortisol, protective bacteria decline). And the dysbiosis that results maintains low-grade systemic inflammation that worsens brain stress.
It’s the vicious intestine-brain circle of burnout. Stress alters the intestine, the inflamed intestine sends alarm signals to the brain via the vagus nerve and pro-inflammatory cytokines, the brain interprets these signals as danger, the reptilian activates, cortisol rises, and the intestine deteriorates further. As I detail in the article on depression and neurotransmitters, intestinal inflammation activates the IDO enzyme that diverts tryptophan from the serotonin pathway toward the kynurenine pathway. Result: less serotonin, more neurotoxic metabolites, and a brain that sinks deeper into anxiety and exhaustion.
This is why the recovery protocol for burnout must include an intestinal component. Intestinal restoration through the 4R protocol (remove, replace, reseed, repair) is an essential pillar. Without a functional intestine, the nutrients you take won’t be absorbed. And without absorption, no neurotransmitter synthesis. It’s that simple and that frustrating.
The case of Thomas: six months to regain control
Thomas’s assessment revealed what I find in the vast majority of my burnout patients. Magnesium levels in red blood cells were collapsed (sign of cellular depletion, not just serum). Serum zinc at the low end of normal. Vitamin D at 18 ng/mL (frank insufficiency). Salivary cortisol showing a typical profile of stage 2-3 adrenal exhaustion: flattened morning cortisol (the adrenals no longer respond to the wake-up demand) and still elevated evening cortisol (the brake no longer works at night). An omega-3 index of 3.8 % (catastrophic for a brain that uses them massively). And ferritin at 28 ng/mL, technically “within normal limits” but far too low to ensure optimal neurotransmitter synthesis.
The protocol lasted six months, structured in three phases.
Phase 1 (months 1-2): put out the fire. Extended leave from work at six weeks (not two weeks, that’s insufficient). Magnesium bisglycinate 400 mg per day. High-dose B complex. Vitamin C 1.5 grams per day. Vitamin D3 4000 IU per day. Omega-3 EPA/DHA 3 grams per day. Melatonin 1 mg at bedtime to restore sleep. Cardiac coherence three times five minutes per day. Daily thirty-minute walk.
Phase 2 (months 3-4): rebuild the foundations. Rhodiola 300 mg in the morning. Zinc bisglycinate 25 mg at bedtime. Iron bisglycinate 30 mg with vitamin C (to raise ferritin above 50). 4R intestinal protocol (L-glutamine, multistrain probiotics, curcumin). Resumption of gentle, regular physical activity. Chrononutrition: protein-rich breakfast (eggs, nuts, avocado) for morning dopamine, complex carbohydrates in the evening to favor tryptophan passage to the brain and serotonin synthesis[^14].
Phase 3 (months 5-6): consolidate and prevent. Gradual reduction of supplements. Maintenance of magnesium and omega-3s long-term. Work on neolimbic patterns (identify inadequate automatic responses, train recourse to the prefrontal). Gradual return to work with a negotiated adjustment (reduced hours, redefined priorities).
At three months, Thomas was sleeping again. At four months, he recovered his concentration. At six months, he told me something that sums up all the work accomplished: “I didn’t change jobs. I changed my brain.” What he meant was that he had learned not to let his reptilian make decisions instead of his prefrontal. And that his body, finally properly nourished, gave him the means again to choose.
The limits of the natural approach
Severe burnout is a medical emergency. If you have dark thoughts, if you can’t get out of bed, if you cry without reason every day, if your HAD score exceeds 15, see a doctor. Micronutrition and naturopathy are powerful but complementary levers. They don’t replace a work leave when it’s necessary, psychiatric follow-up when depression is established, or medical management when the situation requires it.
The question Thomas asked me at our first session, “how did I get here,” has a precise neurobiological answer. He got there because his neolimbic brain treated complex situations for five years with simple responses. Because his prefrontal sent thousands of error signals that were intercepted by his reptilian. Because his reptilian triggered thousands of cortisol cascades that depleted his adrenal glands, his magnesium, his zinc, his B vitamins, his sleep and his joy of living. Burnout is not a lack of willpower. It’s a neurobiological short-circuit on a depleted terrain. And when you understand the mechanism, you understand the solution.
If you recognize yourself in Thomas’s journey, start with the basics of naturopathy to understand the concept of terrain. If you want to explore the connection between your adrenal glands and your thyroid, read the article on stress, cortisol and the thyroid. And if you want to know if your brain is lacking raw materials, the article on depression and neurotransmitters is the natural complement to this one. Your brain is an organ. It is nourished. It repairs itself. And it can relearn to trust its prefrontal rather than its reptilian.
If you want personalized support, you can schedule a consultation.
To go further
- Basedow and stress: the thyroid of emotion
- Holmes-Rahe scale: when life events make you sick
- DHEA: the forgotten hormone of your vitality and immunity
- Adrenal exhaustion: the 3 stages no one explains to you
Want to assess your status? Take the free Holmes Rahe stress questionnaire in 2 minutes.
Want to assess your status? Take the free Hertoghe cortisol questionnaire in 2 minutes.
Sources
- Lucas, Anne. Stress, Anxiété, Burn Out & Micronutrition. Course #24, DU MAPS, 2020.
- Selye, Hans. The Stress of Life. McGraw-Hill, 1956.
- Laborit, Henri. L’inhibition de l’action. Masson, 1986.
- Hertoghe, Thierry. The Hormone Handbook. 2nd ed. International Medical Books, 2012.
“Inhibition of action is the source of anguish. Anguish is the source of all illness.” Henri Laborit
Scientific references
Footnotes
-
Lucas A. Stress, Anxiété, Burn Out & Micronutrition. DU de Micronutrition, Alimentation, Prévention et Santé (MAPS), course #24. Slide on fundamental stress principles: “It is not things themselves that disturb people, but their judgments about those things.” ↩
-
Selye H. A syndrome produced by diverse nocuous agents. Nature 138 (1936): 32. The general adaptation syndrome in three phases: alarm, resistance, exhaustion. ↩
-
Laborit H. L’inhibition de l’action. Masson, 1986. Three states of instinctual emergency: flight, fight, inhibition of action (freeze). ↩
-
Lucas A. DU MAPS, course #24. Slides on the neurocognitive and behavioral approach (ANC): “4 brain territories: reptilian (individual survival, stress), paleolimbic (collective survival, self-affirmation), neolimbic (simple/known, automatic mode), prefrontal neocortex (complex/unknown, adaptive mode).” ↩
-
Lucas A. DU MAPS, course #24. Stress mechanism according to ANC: “New situation perceived as simple by the neolimbic, autopilot, inadequate response, prefrontal detects the error, signal to the reptilian, inappropriate alarm.” ↩
-
Lucas A. DU MAPS, course #24. ANS dysfunction: “Tachycardia, palpitations, hot flushes, muscle tensions, bruxism, sweating, transit problems.” ↩
-
Sapolsky RM. Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Archives of General Psychiatry 57, no. 10 (2000): 925-935. PMID: 11015810. ↩
-
Lucas A. DU MAPS, course #24. HAD questionnaire: “0-7 normal, 8-10 mild, 11-14 moderate, 15-21 severe.” Cohen’s scale: “<25 no stress, 25-49 moderate, >50 pathological.” ↩
-
Holmes TH, Rahe RH. The Social Readjustment Rating Scale. Journal of Psychosomatic Research 11, no. 2 (1967): 213-218. PMID: 6059863. Score >300: 80 % risk of illness within the year. ↩
-
Lucas A. DU MAPS, course #24. The prefrontal neocortex: “Manages the complex and the unknown. Adaptive mode. Open-mindedness, innovation, acceptance of uncertainty. Only territory capable of processing novelty ↩



Laisser un commentaire
Sois le premier à commenter cet article.