Your Digestion Is Not the Problem: Your Thyroid Is
Your meals sit heavy in your stomach? Acid reflux wakes you at night? You feel bloated after every meal, even when you eat “well”? Before rushing to PPIs or Gaviscon, ask yourself a question no one has ever asked you: what if it’s your thyroid?
Hypochlorhydria, the lack of hydrochloric acid in the stomach, is the digestive symptom par excellence of hypothyroidism. Yet it is systematically confused with excess acidity. The trap is formidable: the doctor prescribes a proton pump inhibitor (PPI) that further reduces acidity, which aggravates nutrient malabsorption, which aggravates hypothyroidism, which aggravates hypochlorhydria. The vicious circle is complete.
Paul Carton wrote: “Digestion is a battle.” This phrase has never been more relevant than in thyroid terrain. In consultation, I observe that nearly all of my hypothyroid patients present at least one significant digestive symptom. Some have five or six. And in the vast majority of cases, no one has connected their belly to their thyroid.
The Digestive Tract Under Hypothyroidism
To understand why the thyroid and digestion are so intimately linked, you must return to a fundamental concept: the thyroid regulates the metabolism of every cell in your body. Every cell. Including the cells of your stomach, pancreas, small intestine, and colon. When the thyroid slows down, the entire digestive tract slows down with it.
The first area affected is the stomach. The gastric parietal cells, which produce hydrochloric acid (HCl), depend directly on thyroid stimulation. In hypothyroidism, HCl production decreases progressively. This is hypochlorhydria. Hydrochloric acid is not merely a simple food dissolver. It activates pepsin (the enzyme that digests proteins), it sterilizes the food bolus (barrier against pathogenic bacteria), it stimulates the secretion of bile and pancreatic enzymes downstream, and most importantly it enables the ionization and absorption of minerals. Without sufficient acid, iron, zinc, calcium, magnesium, and vitamin B12 pass through the digestive tract without being absorbed. This is how hypothyroidism creates deficiencies that worsen itself.
The second area is the lower esophageal sphincter. This muscle that closes the entrance to the stomach is sensitive to gastric pH. When acidity is insufficient, the sphincter relaxes. Result: the small amount of acid present rises into the esophagus and causes reflux. This is the paradox I find in almost all my GERD patients: they have reflux not from excess acid, but from deficiency. And the PPIs prescribed to them worsen the underlying problem by reducing acid production even further.
The third area is gastric emptying. Hypothyroidism causes functional gastroparesis: food remains longer in the stomach. Meals that “sit heavy,” the sensation of heaviness, postprandial nausea, all of this reflects a slowing of gastric motility directly linked to T3 deficiency.
The fourth area is the exocrine pancreas. Less thyroid stimulation means less production of pancreatic enzymes (lipase, amylase, protease). Fats, starches, and proteins are incompletely digested. Fatty stools, flatulence after a rich meal, and the sensation of never properly digesting fats are classic signs.
The fifth area is the small intestine. Peristalsis is slowed, the mucosa renews less well, the villi lose absorptive surface. If dysbiosis becomes established (which is common when gastric pH is unbalanced), malabsorption worsens further. Dr Mouton emphasizes the frequent coexistence between intestinal dysbiosis and thyroid insufficiency, which he considers as two facets of the same terrain imbalance. To deepen your understanding of the link between intestine and thyroid auto-immunity, consult my article on Hashimoto.
The sixth area is the colon. Constipation is a cardinal symptom of hypothyroidism. Dr Mouton is categorical: every patient with chronic constipation should first be considered hypothyroid until proven otherwise. He describes extreme cases (one bowel movement per week, every two weeks, even monthly) and warns that these patients are at risk for colorectal, breast, or prostate cancer. Paradoxically, some of these patients alternate between constipation and diarrhea, the only way the body finds to “break the blockage.”
The Vicious Circle
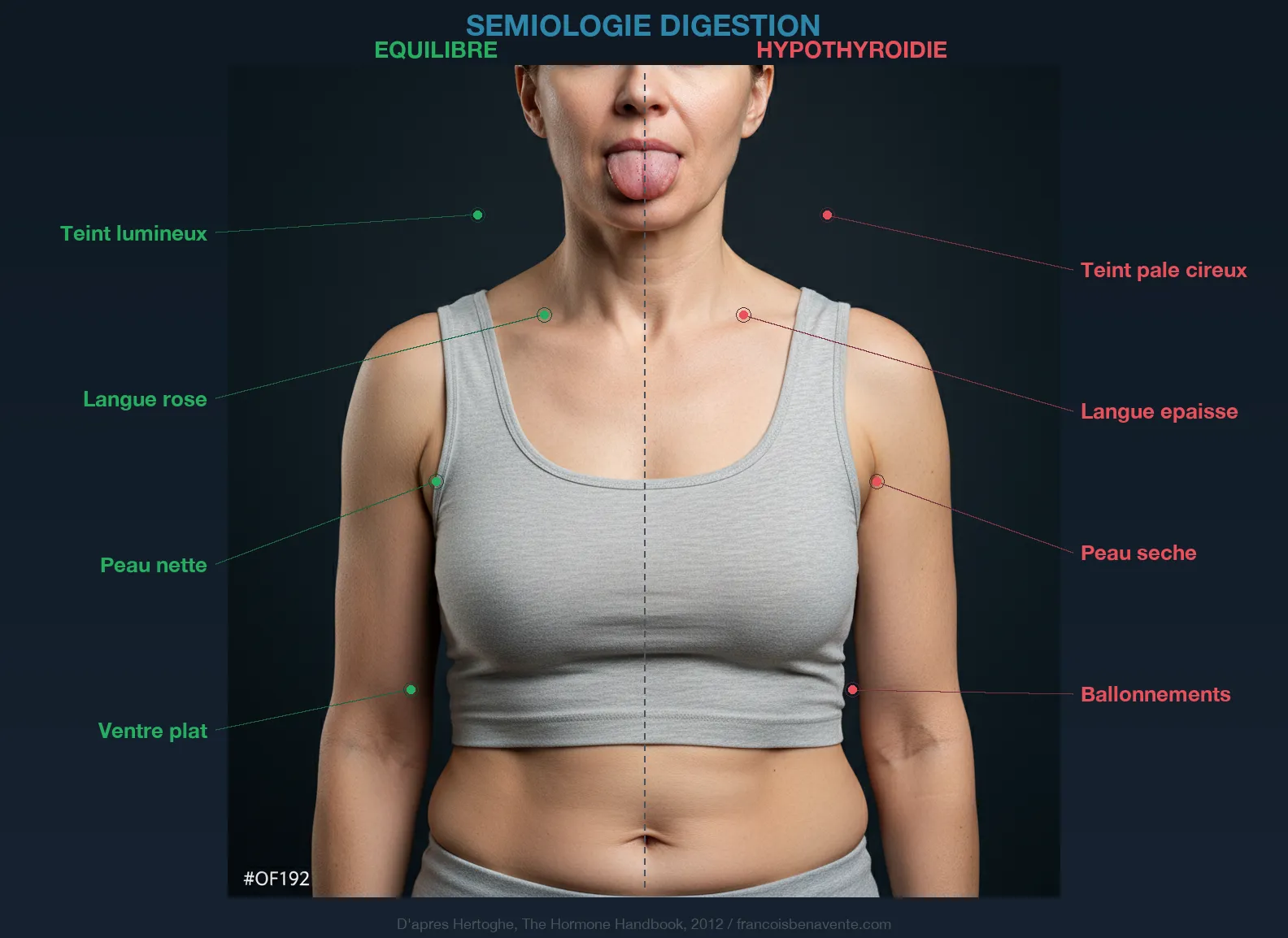
The insidious nature of the thyroid-digestion relationship lies in its circularity. Hypothyroidism causes hypochlorhydria. Hypochlorhydria causes malabsorption of iron, zinc, B12, and selenium. Iron deficiency prevents thyroperoxidase from functioning. Selenium deficiency blocks T4 conversion to T3. Zinc deficiency compromises hormone synthesis and thyroid hormone cellular uptake. Which worsens hypothyroidism. Which worsens hypochlorhydria. And the circle turns.
I have seen patients in consultation take iron capsules for months without their ferritin moving a point. Not because the iron was poor quality, but because their stomach did not produce enough acid to ionize and absorb it. They were supplementing into a void. The iron went from mouth to toilet without stopping. This is why, in my approach, correcting digestion is a prerequisite to any supplementation. If you suffer from anemia resistant to supplementation, the thyroid pathway definitely deserves exploration.
This vicious circle is further aggravated by classically prescribed medications. PPIs (omeprazole, esomeprazole, lansoprazole) reduce acid production by ninety percent. Prescribed initially for reflux, they are often maintained for years. Yet a study published in JAMA showed that prolonged PPI use is associated with increased risk of fractures and deficiencies in B12, magnesium, and iron. Exactly the cofactors the thyroid needs most.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are another frequent aggressor. They increase intestinal permeability (the famous leaky gut) and damage the microbiota. Oral contraceptives decrease zinc and weaken adrenal function. Repeated antibiotics destroy protective Lactobacillus and Bifidobacterium species, promoting the proliferation of Candida albicans and other pathogens. Each of these factors feeds the vicious circle at its level.
The Digestive Impacts of Hypothyroidism
Beyond the digestive tract itself, hypothyroidism impacts three accessory organs that play a major role in digestion.
The liver is the first. It converts sixty percent of T4 to active T3, but it also depends on T3 to function properly. In hypothyroidism, bile production is reduced, cholesterol metabolism is slowed (which explains the frequent high cholesterol in hypothyroid individuals), and hepatic detoxification runs at a crawl. An overloaded liver converts even less T4 to T3, which worsens the digestive picture. This is the concept of “thyroid fatty liver” that I develop in my approach. Hepatic drainage with fresh vegetable juices (carrot, beet, celery, ginger) is a pillar of my strategy.
The gallbladder is the second organ. Bile, produced by the liver and stored in the gallbladder, is essential for fat digestion and absorption of fat-soluble vitamins (A, D, E, K). In hypothyroidism, the gallbladder contracts less vigorously, bile becomes saturated, and gallstones form more easily. If you digest fats poorly, if you have nausea after a fatty meal, or if you have already had gallstones, the thyroid pathway is worth exploring.
The small intestine is the third organ, but also the site of a fundamental bidirectional relationship. The small intestine ensures about twenty percent of T4 to T3 conversion via deiodinases present in the mucosa. An inflamed, permeable, or dysbiotic intestine no longer converts properly. Furthermore, the microbiota regulates thyroid activity directly through the production of metabolites (short-chain fatty acids, B vitamins) and modulation of the immune system. This is why I consider that healing the intestine means healing the thyroid.
Ten Concrete Strategies
Through my consultations, I have refined a set of practical strategies that allow you to break the thyroid-digestion vicious circle. They do not replace correcting thyroid cofactor deficiencies (which I detail in the article on thyroid and micronutrition), but they create the conditions for this correction to be effective.
The first strategy is to stimulate gastric acidity. One teaspoon of apple cider vinegar in a glass of warm water, fifteen minutes before each main meal. You can enhance it with freshly grated ginger and turmeric powder. Ginger is a natural prokinetic that stimulates gastric emptying, while turmeric is anti-inflammatory for the mucosa. This simple vinegared water often dramatically improves digestion within the first few days.
The second strategy is to respect digestion times. Meat requires four hours of digestion, cheese rich in casein requires eight. An egg is digested in one hour, white fish and shellfish in two hours. The fattier a food, the longer it stays in the stomach, with the exception of mono- and polyunsaturated fats (avocado, olive oil, canola oil) which require only about two hours. In hypothyroidism, you should prioritize easily digestible foods, especially in the evening.
The third strategy concerns fruits. They require only thirty minutes of digestion and, through their fructose content, support thyroid function. Fructose is a rapid energy substrate that does not excessively stimulate insulin. Juicy pears, ripe bananas, apples, and persimmons are allies of thyroid terrain. Ideally as snacks, not at the end of a heavy meal where they would ferment.
The fourth strategy is conscious chewing. Chewing slowly, mindfully, in calm, activates the parasympathetic nervous system that governs all digestive secretion (saliva, acid, enzymes, bile). A meal gulped in front of a screen in ten minutes short-circuits this cascade. Eat as if you hadn’t eaten in a long time. This simple advice literally transforms digestion for many of my patients.
The fifth strategy is soaking nuts and pseudo-cereals. Rice, quinoa (two hours soaking), beans (four hours), nuts (four hours) contain anti-nutrients (phytic acid, lectins, enzyme inhibitors) that worsen malabsorption. Soaking with rinsing removes these anti-nutrients and activates the enzymatic potential of the food.
The sixth strategy is to split meals. Rather than three large meals that overload a slowed digestive system, eat four to five small meals to lighten the load at each intake. The protein-rich breakfast (eggs, avocado, soaked nuts) provides hormone precursors. Dinner should be light and taken early so you don’t lie down with a full stomach.
The seventh strategy is targeted enzymatic support. Vegetable digestive enzymes (bromelain, papain) or betaine HCl (under a practitioner’s supervision) can compensate for hypochlorhydria while the thyroid recovers. Anise seeds, fennel, fresh fenugreek sprouts or powder enhance meals while supporting digestive secretion.
The eighth strategy is to nourish the microbiota. Raw and cooked vegetables (prebiotics) to feed the good bacteria. The most documented strains for intestinal and thyroid health are Lactobacillus rhamnosus, Lactobacillus gasseri, and Bifidobacterium bifidum. Inulin (present in garlic, onion, artichoke, chicory) favors the growth of Akkermansia muciniphila, a bacterium associated with better metabolic health.
The ninth strategy is glutamine. This amino acid is the primary fuel for intestinal cells (enterocytes). Four to eight grams per day helps repair the mucosa and restore intestinal permeability. Glutamine is particularly indicated when leaky gut coexists with hypothyroidism, which is the case in most auto-immune situations.
The tenth strategy is gentle liver drainage. Vegetable-based dinners (green vegetables, vegetable soups) two to three evenings per week, fresh vegetable juices in the morning (carrot, beet, celery, ginger), and hepatic herbs (milk thistle, artichoke, rosemary) support the function of T4 to T3 conversion and improve bile production. If you want to go further with detoxification, my article on spring detox proposes a complete protocol.
The Intestine, Gateway to the Thyroid
The relationship between the intestine and the thyroid goes far beyond simple malabsorption. The intestine houses seventy percent of the immune system. Intestinal dysbiosis (flora imbalance) disrupts the balance between Th1 and Th2 lymphocytes, which can trigger or worsen auto-immune thyroiditis. Dr Mouton has identified the frequent coexistence between fungal dysbiosis (intestinal candidiasis) and thyroid insufficiency, which he considers as two major sources of immune deficiency.
The neurological symptoms of dysbiosis (anxiety, fatigue, depression, mood changes, memory loss, insomnia) are strangely similar to those of hypothyroidism. This overlap is not coincidence. Mycotoxins produced by intestinal yeasts (particularly Candida albicans) act directly on the nervous system, just as T3 deficiency acts on the brain. When both coexist, neuropsychological symptoms are amplified and difficult to untangle.
Dietary tryptophan, metabolized by the microbiota into indole derivatives and kynurenine, favors the differentiation of regulatory T lymphocytes (Treg). These cells are the guardians of immune tolerance: they prevent the immune system from attacking the body’s own tissues. When the flora is altered, Tregs decrease, and autoimmune risk increases. This is a crucial mechanism that directly links intestinal health to thyroid health. To understand tryptophan’s role in serotonin production and its link to the thyroid, consult the dedicated article.
Arginine and glutamine are true reconstructors of the intestinal mucosa. Arginine also plays an antimicrobial immune role by regulating macrophage activity. Omega-3s (fish oil, flaxseed oil, walnuts, canola) improve the flexibility of intestinal cell membranes and could modulate probiotic adhesion to the mucosa.
When to Consult
If you recognize yourself in several of the symptoms described in this article, the first step is to verify your thyroid function with a complete panel (not just TSH). The article on hypothyroidism as a symptom details the five upstream causes to explore and Hertoghe’s self-assessment questionnaire.
The digestive panel should include, at minimum, a urinary organic metabolites test (MOU) if dysbiosis is suspected, a ferritin level (functional target 50 to 80 ng/mL), active B12, serum zinc, and if possible an IgG food test to identify specific intolerances beyond gluten and casein.
Remember that Levothyrox itself is sensitive to your digestive tract’s state. Coffee taken less than thirty minutes after the tablet reduces its absorption. PPIs interfere with its assimilation. And an inflamed intestinal mucosa absorbs the medication less well, which may explain why some patients don’t respond to their prescribed dose.
The good news is that this vicious circle can become a virtuous circle. When digestion improves, cofactor absorption increases. When cofactors are better absorbed, the thyroid functions better. When the thyroid functions better, digestion improves again. The first step is to break the circle somewhere, anywhere, and let the positive cascade unfold.
Want to evaluate your status? Take the free Claeys thyroid questionnaire in 2 minutes.
If you want personalized support, you can book a consultation.
To Go Further
- Hypothyroidism is a symptom, not a diagnosis
- Magnesium: why your thyroid, sleep, and stress depend on it
- Hertoghe Diet: the dietary protocol that optimizes your thyroid
- Thyroid: the 7 nutrients your endocrinologist never measures
Sources
- Carton, Paul. Treatise on Medicine, Nutrition and Natural Hygiene. Paris: Librairie Le François, 1920.
- Mouton, Georges. Digestive Ecology. Marco Pietteur, 2004.
To sleep well and support the foundations of naturopathy, consult the dedicated articles. And if you need personalized support to untangle your thyroid and digestive situation, you can book a consultation.
Based in Paris, I consult via video throughout France. For quality digestive enzymes and probiotic supplementation, Sunday Natural (-10% with code FRANCOIS10). The juice extractor remains an indispensable tool for preparing fresh vegetable juices that support the liver and thyroid daily.
Healthy Recipe: Regenerating bone broth: Bone broth repairs the digestive mucosa.






Laisser un commentaire
Sois le premier à commenter cet article.