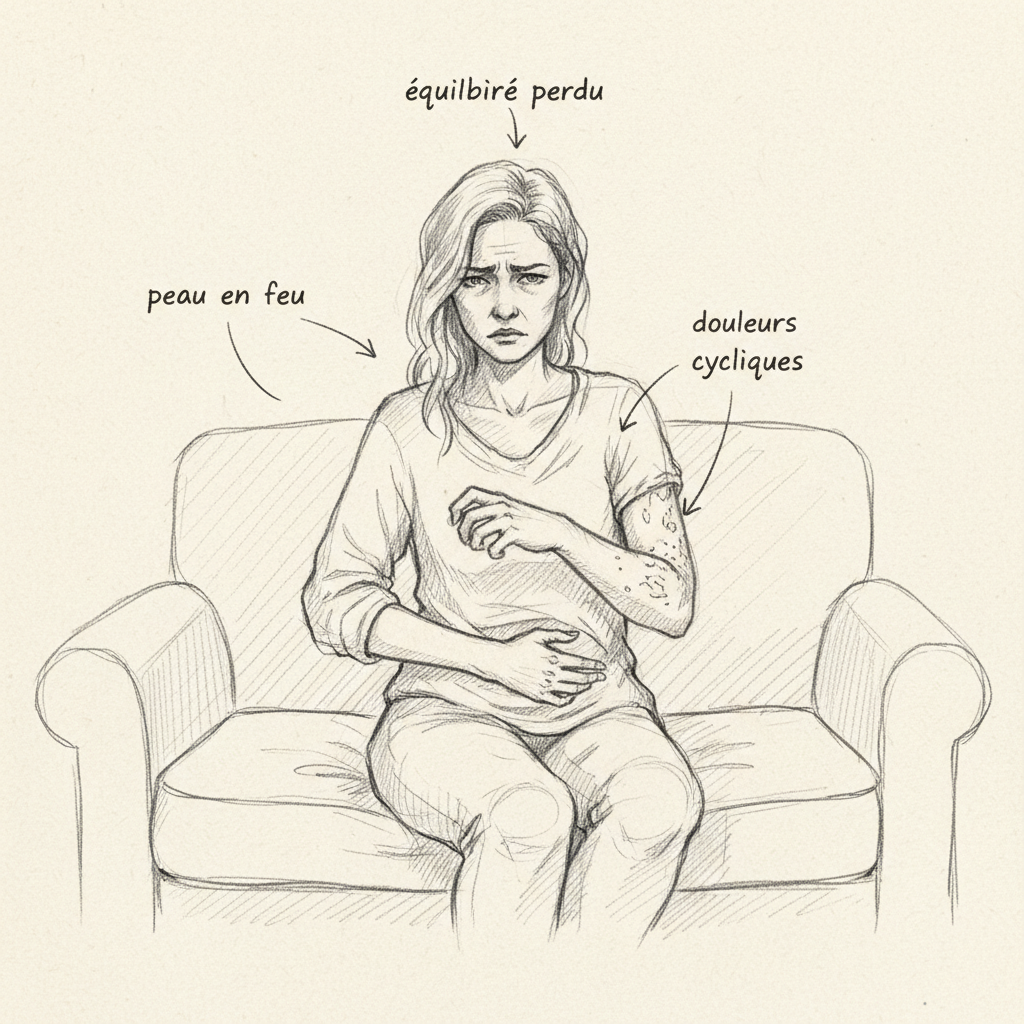
Her name is Nathalie (name changed), 38 years old, two children. When she sat down across from me, her hand skin was so dry it was flaking in patches, her breasts had been tender for ten days, and she had that irritable fatigue I now recognize at first glance. “I’m unmanageable a week before my period. My husband says I become a different person. And my skin, look at it, no cream works.” I asked her how long this had been happening. “Since forever for the skin. Since my second pregnancy for the rest. My dermatologist says it’s constitutional eczema, my gynecologist offers me the pill for PMS, and my GP tells me to drink more water.”
I looked at her elbows. Rough, keratotic patches, typical of xerosis. The outer surface of her arms, riddled with small granular papules: keratosis pilaris. Striated nails, brittle hair. And especially, when I asked if she ate fatty fish, she gave me that answer I hear three times a week: “Not really, no.” When I asked about the oils in her kitchen, she said sunflower. When I asked about supplements, she said none.
“The body doesn’t cry out randomly. Every symptom is a message. Dry skin, menstrual pain, irritability: three signals, one single deficiency.” Dr Jean-Paul Curtay, Nutritherapy
The tests I ordered confirmed what semiology suggested: a red blood cell fatty acid profile collapsed in GLA (gamma-linolenic acid), DGLA (dihomo-gamma-linolenic acid) at floor level, and an omega-6/omega-3 ratio of 18 to 1. Nathalie wasn’t lacking omega-6, she had far too much in the form of linoleic acid. What she lacked was the ability to convert it. Her enzymatic motor was stuck. And no one had ever explained this to her.
The causes of GLA deficiency
To understand why GLA is so often lacking, you first need to understand the omega-6 cascade. It’s a biochemical chain in several steps, and the slightest break at any link has downstream consequences.
It all starts with linoleic acid (LA, C18:2 n-6), an essential fatty acid with eighteen carbons and two double bonds. Essential means the body can’t make it: it must absolutely come from food. Linoleic acid is abundant in modern diets, often even in excess (sunflower, corn, soy oils, processed foods). So far, no problem. The problem begins at the next step.
Linoleic acid must be converted to GLA (gamma-linolenic acid, C18:3 n-6) by an enzyme called delta-6-desaturase (D6D). This enzyme adds a third double bond at carbon 6 of the chain. It’s the rate-limiting step of the entire cascade1. If this enzyme doesn’t work correctly, the entire rest of the chain collapses, regardless of how much linoleic acid is in the diet. This is exactly what happens to millions of people without them knowing it. David Horrobin, the researcher who studied GLA most extensively throughout his career, devoted thirty years to documenting this enzymatic bottleneck. His work published in 2000 in the American Journal of Clinical Nutrition remains the reference2.
GLA is then elongated to DGLA (dihomo-gamma-linolenic acid, C20:3 n-6) by an elongase. This step is rapid and rarely rate-limiting. DGLA is the true hero of this story, because it’s the direct precursor of anti-inflammatory PGE1 prostaglandins, vasodilators, platelet anti-aggregants and immunomodulators. PGE1 is the exact counterweight to PGE2, those pro-inflammatory prostaglandins that cause menstrual pain, joint stiffness, water retention, breast tension.
DGLA can then be converted to arachidonic acid (AA, C20:4 n-6) by delta-5-desaturase. And this is where the surrounding discourse becomes muddled. Arachidonic acid is the precursor of pro-inflammatory series 2 eicosanoids: PGE2, thromboxane A2, leukotrienes LTB43. This is why you hear everywhere that omega-6s are “bad” and “pro-inflammatory.” But this is a dangerous shortcut. The reality is that the omega-6 cascade produces both anti-inflammatory mediators (PGE1, via DGLA) and pro-inflammatory ones (PGE2, via AA). Everything depends on where the cascade stops, and on available cofactors. When D6D is blocked, DGLA doesn’t form, PGE1 isn’t produced, and excess linoleic acid takes oxidative pathways that feed low-grade inflammation. It’s the worst of both worlds.
Professor Gérard Mouton, in Intestinal Ecosystem and Optimal Health, emphasizes a point most practitioners ignore: DGLA is not only a PGE1 precursor, it’s also a competitive inhibitor of the conversion of arachidonic acid to PGE2. In other words, the more DGLA you have, the less pro-inflammatory PGE2 you produce. GLA thus has a double anti-inflammatory effect: it increases PGE1 production and slows PGE2 production. This is what Horrobin called the “omega-6 paradox”: supplementing with GLA decreases inflammation instead of aggravating it.
The factors that inhibit delta-6-desaturase are terrifyingly common in the modern lifestyle. Aging is the first: after age 40, D6D activity gradually decreases, which partly explains the dry skin, joint stiffness and low-grade inflammation that accompany aging4. Diabetes and insulin resistance powerfully block D6D, creating a metabolic vicious circle. Alcohol is a direct and dose-dependent inhibitor. Trans fatty acids (hydrogenated margarines, industrial pastries, deep fryers) bind to the enzyme’s active site and prevent it from functioning. Chronic stress, via cortisol, slows enzymatic activity. And cofactor deficiencies (zinc, magnesium, vitamin B6, iron) deprive the enzyme of its tools. Dr Jean-Paul Curtay, in Nutritherapy, summarizes the situation forcefully: “Delta-6-desaturase is the most fragile enzyme in lipid metabolism. Everything conspires to block it.”
Symptoms of deficiency
GLA and DGLA deficiency manifests as a recognizable clinical picture in consultation, if you know where to look. It’s a terrain of dryness, inflammation and hormonal imbalance that affects multiple systems at once.
The skin speaks first. Diffuse dry skin, resistant to even the richest moisturizing creams, is the most common sign. Keratosis pilaris (those little granular papules on the outer surface of the arms, sometimes the thighs and buttocks) is a classic marker of essential fatty acid deficiency. Horrobin was the first to demonstrate that patients with atopic eczema have a constitutional deficiency in delta-6-desaturase5. Their skin can’t convert linoleic acid to GLA, which deprives the epidermis of the ceramides necessary for barrier function. Lips crack, heels become fissured, nails become brittle and dry hair loses its shine. All of this tells the same story: a deficiency in long-chain polyunsaturated fatty acids at the membrane level.
Atopic eczema deserves special attention. Several studies have shown that atopic infants have plasma GLA and DGLA levels significantly lower than non-atopic infants, even with normal linoleic acid intake5. This is proof of a constitutional enzymatic blockage. GLA supplementation (evening primrose or borage oil) has shown variable but significant clinical results in some studies, particularly in children with very low baseline DGLA levels.
Premenstrual syndrome (PMS) is the second major territory of GLA deficiency. Cyclical mastalgia (breast tension and pain in the second half of the cycle), premenstrual irritability, water retention, bloating, sugar cravings, mood disturbances: this whole array of symptoms is linked to a prostaglandin imbalance. Pruthi and colleagues’ work at the Mayo Clinic confirmed the effectiveness of evening primrose oil on cyclical mastalgia6. The mechanism is clear: GLA increases PGE1 production, which directly opposes the effects of prolactin on breast tissue. When PGE1 is insufficient, prolactin causes breast hypersensitivity that many women know all too well. If your periods are painful in addition to being accompanied by breast tension, GLA deficiency is a major lead to explore.
Mucosal dryness is a less well-known but very revealing sign. Dry eyes (dry eye syndrome), vaginal dryness (outside of menopause), dry mouth are possible manifestations of long-chain essential fatty acid deficiency. PGE1 plays a role in regulating mucous secretions, and their deficiency leads to reduced mucus and tear production.
Diabetic neuropathy is an area where GLA has been the subject of promising research. Diabetes inhibits D6D, which reduces GLA and DGLA production, which decreases the PGE1 necessary for microcirculation of the vasa nervorum (the small vessels that irrigate peripheral nerves). The result: progressive deterioration of nerve conduction. Horrobin and colleagues showed that GLA supplementation at a dose of 480 mg per day for one year significantly improved nerve conduction scores in diabetic patients7. It’s one of the rare areas where GLA has been the subject of a large-scale, double-blind, randomized clinical trial.
Inflammatory joint disorders are another possible manifestation. Deficiency in anti-inflammatory PGE1, combined with excess arachidonic acid and PGE2, promotes morning stiffness, joint pain and chronic joint inflammation. Rheumatoid arthritis has been the subject of several studies with high-dose borage oil, with significant results in reducing pain and stiffness8.
Essential micronutrients for omega-6
Delta-6-desaturase doesn’t work alone. It needs a team of cofactors to do its job. Without them, even optimal linoleic acid intake won’t produce GLA. This is a fundamental point that most prescribers neglect: prescribing evening primrose oil without checking cofactors is like ordering firewood without having a fireplace.
Zinc is the number one cofactor for D6D. Each delta-6-desaturase molecule contains a zinc atom in its catalytic site. In zinc deficiency, the enzyme slows down or stops. Yet zinc is the trace element whose deficiency is most common in the Western population. The two deficiencies (zinc and GLA) reinforce each other mutually in a silent vicious circle. Curtay emphasizes that correcting zinc is often the first step in restarting the omega-6 cascade.
Magnesium is the second critical cofactor. It intervenes in D6D function and in over 300 enzymatic reactions. Magnesium deficiency affects approximately 70% of French people according to the SU.VI.MAX study. It aggravates stress (magnesium is the physiological anti-stress), which itself inhibits D6D. This is another vicious circle.
Vitamin B6 (pyridoxine, and especially its active form pyridoxal-5-phosphate or P5P) is essential for the functioning of desaturases and elongases. B6 is also the cofactor for serotonin synthesis, which explains why B6 deficiency causes both mood disturbances and skin disorders. Women on hormonal contraceptives are particularly at risk of B6 deficiency, because synthetic estrogens increase P5P degradation. This is a detail few gynecologists mention.
Iron acts as a cofactor in the desaturation reaction, just like zinc. Iron-deficiency anemia or even iron deficiency without anemia (low ferritin with normal hemoglobin) can compromise the conversion of linoleic acid to GLA. This is a particularly relevant point in women of childbearing age, who often cumulate iron deficiency, zinc deficiency, and symptoms of GLA deficiency (PMS, dry skin, eczema).
Vitamin B3 (niacin) also participates in desaturase function via NADH. Vitamin C plays a protective role by preserving polyunsaturated fatty acids from oxidation. And biotin (vitamin B8) intervenes in overall lipid metabolism. A terrain deficient in several of these cofactors simultaneously, which is extremely common in modern diets, creates the perfect conditions for D6D blockage. This is why Dr Thierry Hertoghe, in The Hormone Handbook, always recommends a complete micronutritional assessment before any targeted supplementation: “Correcting one nutrient in isolation without looking at the terrain is repainting a cracking wall.”
Dietary sources
GLA is a fatty acid that common diets provide virtually no amount of as such. Unlike linoleic acid, which is omnipresent in vegetable oils, GLA is found in significant amounts only in a few specific sources. This is why supplementation is often necessary when D6D is deficient.
Borage oil (Borago officinalis) is the most concentrated source of GLA at 20 to 24% of its fatty acid composition. One gram of borage oil therefore provides 200 to 240 mg of GLA. It’s the source of choice when you want maximum intake with minimal capsules. Borage is a Mediterranean plant that herbalists have used for centuries for skin and mucous membranes, long before we understood GLA’s biochemistry.
Evening primrose oil (Oenothera biennis) contains 8 to 10% GLA. One gram of evening primrose oil therefore provides 80 to 100 mg of GLA. It’s the most clinically studied source, with decades of publications on PMS, atopic eczema and mastalgia. Evening primrose (primrose of the evening, or evening primrose in English) is a North American plant whose tiny seeds are cold-pressed to extract the oil. It also contains approximately 72% linoleic acid, making it a very rich omega-6 oil in the broad sense.
Black currant seed oil (Ribes nigrum) is an underappreciated source worth exploring. It contains approximately 15 to 17% GLA, but also stearidonic acid (C18:4 n-3), an omega-3 intermediate between ALA and EPA. It’s the only oil that provides both an anti-inflammatory precursor of the omega-6 series (GLA) and a precursor of the omega-3 series. For this reason, some practitioners consider it the most balanced source.
On the daily diet side, linoleic acid (the GLA precursor) is abundant in sunflower seeds (approximately 48 g AL per 100 g), walnuts (approximately 38 g/100 g), hemp seeds (approximately 28 g/100 g, with an additional 2 to 4% GLA directly), sesame seeds (approximately 21 g/100 g) and the corresponding oils. But let’s remember: linoleic acid is useless if D6D doesn’t work. And in the modern Western diet, the problem is never a lack of linoleic acid, but rather its relative excess compared to omega-3s, combined with an enzymatic inability to convert it to GLA. This is why supplementation with preformed GLA (evening primrose, borage) is so often necessary: it bypasses the blocked step.
Breast milk is rich in GLA, which is a remarkable evolutionary clue. The infant, whose enzymatic systems are immature, receives GLA directly via their mother’s milk, without needing to make it. When breastfeeding is impossible or insufficient, infant formulas often provide only linoleic acid, which some researchers consider a risk factor in the development of atopic eczema in infants.
Omega-6 antagonists
Knowing what to eat isn’t enough if you don’t know what to avoid. In naturopathy, we always start by removing obstacles before adding solutions. And the obstacles to converting omega-6 to GLA are numerous and omnipresent.
Trans fatty acids are enemy number one. These artificial fatty acids, produced by partial hydrogenation of vegetable oils, have a molecular configuration that allows them to bind to the active site of delta-6-desaturase without being converted. They block the enzyme like a false key in a lock. Hydrogenated margarines, industrial pastries, biscuits, deep-fried foods, prepared meals still contain them despite recent regulations. Curtay reminds us that trans fatty acids don’t just block D6D: they incorporate into cell membranes in place of normal unsaturated fatty acids, stiffening the membrane and disrupting all cellular communication.
Alcohol is a direct and dose-dependent inhibitor of D6D. Even moderate but regular consumption reduces enzymatic activity. It’s one of the mechanisms by which chronic alcohol promotes inflammation, fatty liver, and skin disorders. Horrobin showed that chronic alcoholics have collapsed GLA and DGLA levels, even with sufficient linoleic acid intake2.
Diabetes and insulin resistance powerfully block D6D. Chronic hyperinsulinism disrupts lipid metabolism at several levels, and D6D blockage is one of the most important mechanisms. It’s a vicious circle: diabetes prevents GLA production, which reduces the PGE1 necessary for microcirculation, which worsens diabetes’s vascular complications. Diabetic neuropathy is partly a consequence of this blockage.
Aging progressively slows the activity of all desaturases. After age 40, the capacity to convert linoleic acid to GLA decreases significantly. This is one of the reasons skin dries out with age, joints become stiffer, and low-grade inflammation sets in. Hertoghe, in his work on hormonal aging, emphasizes that GLA deficiency is an underrecognized marker of biological aging.
Cofactor deficiencies (zinc, magnesium, B6, iron) have been detailed in the previous section. Their effect is cumulative and synergistic: each deficiency reduces D6D activity a bit more, and they’re rarely isolated. A patient deficient in zinc is often also deficient in magnesium and B6. It’s the classic picture of deficient terrain that Marchesseau described in his naturopathy lectures.
Excess omega-3 at very high doses is a paradoxical antagonist worth mentioning. Omega-3s (ALA, EPA, DHA) and omega-6s (LA, GLA, AA) share the same conversion enzymes (D6D, D5D, elongases). Massive omega-3 supplementation (beyond 4 to 5 grams per day of EPA+DHA) can, through enzymatic competition, further reduce omega-6 conversion to GLA. This is why some patients taking very high doses of omega-3 paradoxically develop dry skin. Balance, always balance. It’s the very principle of naturopathy.
Chronic stress deserves special mention. Cortisol, the stress hormone, directly inhibits D6D. But stress also acts indirectly: it increases magnesium consumption (increased urinary loss), disrupts blood sugar (stress insulin resistance), disrupts digestion (cofactor malabsorption), and promotes compensatory behaviors (alcohol, sugar, tobacco) that worsen enzymatic blockage. Stress is the systemic inhibitor par excellence of the omega-6 cascade.
Forgotten causes of deficiency
Beyond classic D6D inhibitors, there are more subtle causes that conventional medicine practically never searches for.
Hypothyroidism is probably the most important forgotten cause. The thyroid regulates the baseline metabolism of every cell, including desaturase enzymatic activity. In hypothyroidism, even subclinical (high-normal TSH, low T3), D6D activity decreases significantly. This is one reason why hypothyroid patients often have dry skin, brittle hair and fragile nails, symptoms classically attributed to hypothyroidism itself but actually mediated partly by secondary GLA deficiency from enzymatic slowdown. Hertoghe regularly emphasizes this point: correcting the thyroid also restarts desaturases.
Intestinal dysbiosis is another neglected cause. The intestinal microbiota participates in fatty acid metabolism, and certain bacterial species modulate the expression of desaturase genes in enterocytes. Chronic dysbiosis, candidiasis, intestinal permeability can compromise the bioavailability of essential fatty acids and their cofactors, even with correct dietary intake.
FADS2 gene polymorphism is an exciting lead. The FADS2 gene codes for delta-6-desaturase. Certain polymorphisms of this gene constitutionally reduce enzymatic activity. This is probably the mechanism explaining why atopic eczema is familial: atopic patients inherit a less efficient D6D. This polymorphism was identified as an independent risk factor for eczema, asthma and allergies in several cohort studies9.
Vitamin D deficiency could play a modulatory role, although data is still preliminary. Vitamin D regulates the expression of many lipid metabolism enzymes, and some studies suggest a link between vitamin D status and desaturase activity. This is a rapidly expanding research field.
Finally, tobacco is an often underestimated D6D inhibitor. Nicotine and heavy metals in cigarette smoke disrupt essential fatty acid metabolism at several levels. It’s one reason smokers often have drier, more wrinkled, duller skin than non-smokers, independent of nicotine’s direct vasoconstrictive effect.
Dietary supplements
When D6D is blocked (which is the case for most patients I see in consultation), supplementation with preformed GLA is the most direct solution. We bypass the defective enzyme by providing directly the product it should make.
Evening primrose oil is the most studied and most prescribed supplement. The capsules typically contain 500 mg or 1000 mg of evening primrose oil, of which 8 to 10% is GLA. That’s 40 to 100 mg of GLA per capsule. For premenstrual syndrome, studies use doses of 2 to 3 grams of evening primrose oil per day, or 160 to 300 mg of GLA6. The protocol I use in consultation for PMS is as follows: start supplementation on day 14 of the cycle (after ovulation) and continue until menstruation. This targeting in the second half of the cycle corresponds to the luteal phase, during which PGE1 needs are highest to counterbalance the effects of progesterone drop.
Borage oil is more concentrated in GLA (20 to 24%), which reduces the number of capsules needed. One 1000 mg capsule of borage oil provides 200 to 240 mg of GLA, equivalent to two to three evening primrose capsules. This is the option I favor in patients who struggle swallowing many capsules or who need high GLA doses (severe atopic eczema, rheumatoid arthritis).
Black currant seed oil is a third interesting option, particularly for patients presenting with both GLA deficiency and omega-3 deficiency. Its fatty acid profile is the most balanced of the three sources.
Optimal GLA dosage depends on the indication. For dry skin and keratosis pilaris, 150 to 200 mg of GLA per day generally suffices. For premenstrual syndrome, 200 to 300 mg per day in the luteal phase. For atopic eczema, studies use GLA doses of 300 to 500 mg per day. For diabetic neuropathy, Horrobin used 480 mg per day in his clinical trial. For rheumatoid arthritis, studies with borage oil use doses of 1.4 to 2.8 grams of GLA per day8.
An essential point: GLA supplementation should always be accompanied by its cofactors. A complex containing zinc bisglycinate (15 to 30 mg), magnesium bisglycinate (300 to 400 mg), vitamin B6 in P5P form (25 to 50 mg) and iron bisglycinate if necessary (14 to 28 mg, only if documented deficiency) considerably potentiates GLA’s effect. Without cofactors, some of the supplemented GLA won’t be properly metabolized to DGLA then to PGE1.
GLA supplementation is perfectly compatible with omega-3 supplementation (EPA+DHA). The two fatty acid families produce anti-inflammatory prostaglandins (PGE1 for omega-6s via DGLA, PGE3 for omega-3s via EPA). They’re complementary, not antagonistic. The only case requiring caution is very high-dose omega-3 supplementation (beyond 4 g EPA+DHA per day), which can through enzymatic competition reduce GLA conversion to DGLA. In this case, increasing the GLA dose more than compensates.
GLA supplementation effects aren’t immediate. Expect 6 to 8 weeks to observe initial skin effects, and 2 to 3 cycles for PMS effects. Fatty acids gradually incorporate into cell membranes and tissue phospholipids, and this renewal takes time. This is a point I emphasize strongly in consultation, because many patients give up after two weeks thinking it doesn’t work.
A few precautions to mention. Evening primrose oil and borage oil can slightly lower the epileptic threshold. In epilepsy, supplementation should be discussed with the neurologist. They also have a slight anticoagulant effect (via PGE1), which contraindicates their association with oral anticoagulants without medical advice. And during pregnancy, evening primrose oil is traditionally used late in pregnancy (last month) to prepare the cervix, but it’s inadvisable before the third trimester.
Back to Nathalie. After three months of protocol (borage oil 1000 mg per day or 220 mg of GLA, zinc bisglycinate 25 mg, magnesium bisglycinate 400 mg, vitamin B6 P5P 50 mg, and drastic reduction of sunflower oil in favor of olive oil and small fatty fish), the results were there. The keratosis pilaris on her arms had almost disappeared. Her hand skin no longer flaked. Premenstrual breast tension had decreased by half. And especially, her husband confirmed at the follow-up consultation: “She’s becoming bearable again.” The control red blood cell fatty acid profile showed GLA and DGLA improvement, and the omega-6/omega-3 ratio had dropped to 6 to 1. We were on the right track.
Want to assess your risk of essential fatty acid deficiency? Take the omega-6 deficiency questionnaire in 2 minutes. And if you also suspect an associated thyroid problem, the Claeys test completes the assessment.
For GLA supplementation, Sunday Natural offers pharmaceutical-grade evening primrose and borage oil, cold-pressed and dosed with precision (-10% with code FRANCOIS10). Find all my partnerships with exclusive promo codes.
To go further
- Acetylcholine: the forgotten neurotransmitter of your memory
- Oxidative balance: Dr Brack’s test to measure your oxidative stress
- Cancer and diet: what micronutrition changes in the equation
- Carnitine and thyroid: the molecule no one tests
Sources
- Curtay, Jean-Paul. Nutritherapy. Marco Pietteur, 2016.
- Hertoghe, Thierry. The Hormone Handbook. 2nd ed. Luxembourg: International Medical Books, 2012.
- Horrobin, David F. “Essential Fatty Acid Metabolism and Its Modification in Atopic Eczema.” American Journal of Clinical Nutrition 71, no. 1 (2000): 367s-372s.
- Mouton, Georges. Digestive Ecology. Marco Pietteur, 2004.
“Disease is not an enemy to fight. It’s a signal to understand. The body never makes mistakes in its symptoms.” Pierre-Valentin Marchesseau
Scientific references
Footnotes
-
Nakamura, Manabu T., and Tatsuya Y. Nara. “Structure, Function, and Dietary Regulation of Delta-6, Delta-5, and Delta-9 Desaturases.” Annual Review of Nutrition 24 (2004): 345-376. PMID: 15189125. ↩
-
Horrobin, David F. “Essential Fatty Acid Metabolism and Its Modification in Atopic Eczema.” American Journal of Clinical Nutrition 71, no. 1 (2000): 367s-372s. PMID: 10617999. ↩ ↩2
-
Calder, Philip C. “Eicosanoids.” Essays in Biochemistry 64, no. 3 (2020): 423-441. PMID: 32808660. ↩
-
Cho, Hee Pook, Manabu T. Nakamura, and Steven D. Clarke. “Cloning, Expression, and Fatty Acid Regulation of the Human Delta-5 Desaturase.” Journal of Biological Chemistry 274, no. 52 (1999): 37335-37339. PMID: 10601301. ↩
-
Manku, Mehar S., et al. “Essential Fatty Acids in the Plasma Phospholipids of Patients with Atopic Eczema.” British Journal of Dermatology 110, no. 6 (1984): 643-648. PMID: 6329005. ↩ ↩2
-
Pruthi, Sandhya, et al. “Vitamin E and Evening Primrose Oil for Management of Cyclical Mastalgia: A Randomized Pilot Study.” Alternative Medicine Review 15, no. 1 (2010): 59-67. PMID: 20359269. ↩ ↩2
-
Keen, Harry, et al. “Treatment of Diabetic Neuropathy with Gamma-Linolenic Acid.” Diabetes Care 16, no. 1 (1993): 8-15. PMID: 8380713. ↩
-
Leventhal, Leslie J., Edwin G. Boyce, and Robert B. Zurier. “Treatment of Rheumatoid Arthritis with Gammalinolenic Acid.” Annals of Internal Medicine 119, no. 9 (1993): 867-873. PMID: 8214998. ↩ ↩2
-
Lattka, Eva, et al. “Genetic Variants of the FADS1 FADS2 Gene Cluster as Related to Essential Fatty Acid Metabolism.” Current Opinion in Lipidology 21, no. 1 (2010): 64-69. PMID: 19809313. ↩





Laisser un commentaire
Sois le premier à commenter cet article.